Why NPUAP’s 2016 Terminology Shift Still Matters Legally in 2025
Why NPUAP’s 2016 Terminology Shift Still Matters Legally in 2025
In April 2016, the National Pressure Ulcer Advisory Panel (NPUAP) issued a watershed press release: as of April 13, the term “pressure injury” officially replaced “pressure ulcer” in its staging system, accompanied by expanded and clarified staging definitions—including Medical Device-Related Pressure Injury and Mucosal Membrane Pressure Injury.

While the change in terminology might appear semantic, it carries significant ongoing legal and clinical implications—especially now in 2025, as guidelines evolve and litigation remains a challenge in healthcare settings.
Why the Terminology Shift Matters Legally Today
The term “injury” better captures the pathophysiology—especially for Stage 1 and deep tissue damage, which may not present as ulcers, and may involve still-intact skin. When healthcare providers use accurate language aligned with consensus guidance, documentation becomes more defensible.
Greater clinical precision reduces legal risk
In legal disputes, demonstrating adherence to the precise NPUAP definitions—rather than outdated terms—can help show compliance with the standard of care.
Expanded categories reflect real-world complexity
Incorporating Medical Device-Related Pressure Injury and Mucosal Membrane Pressure Injury into the staging system made the definitions more comprehensive and clinically realistic. In today’s litigation (2025), common claims involve device-related injuries—such as CPAP masks, tracheostomy tie-downs, or endotracheal tubes. Having these classifications recognized in the authoritative staging system arms providers with clearer documentation and defense when such injuries occur.
Continued Evolution: Why 2016’s Foundations Still Matter in 2025
Since 2019, the NPUAP (now NPIAP) has been closely collaborating with international groups to develop evolving clinical practice guidelines. In February 2025, they launched a new “living guideline”, with continuous updates available at the International Guideline website. This living model means that the 2016 terminological update remains a foundational reference. Legal preparedness now must also include a commitment to monitoring guideline changes and updating documentation accordingly.
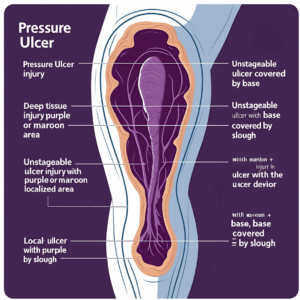
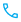
Educational tools still emphasize 2016 staging
Illustrations and training materials based on the 2016 definitions remain widely used in industry and educational settings—freely available through NPUAP resources. Their continued use reaffirms the lasting influence of the 2016 change on professional standards. In legal reviews, providers can show that their staff training adopted these illustrations, reinforcing standard-of-care defenses.
What Legal Practitioners Should Watch in 2025
- Audit clinical documentation language
Ensure that electronic records, charting templates, incident reports, and educational materials use “pressure injury,” not “pressure ulcer,” and reflect staging updates (including DTPI, MDR-PI, mucosal injuries). - Train staff on device-related injury documentation
Legal scrutiny today often zeroes in on injuries from devices. Staff must accurately document the device, staging, preventive actions, and differentiate from other skin damage types. - Embed updates from the living guideline
With the living guideline launched in early 2025, legal risk rises if providers rely solely on pre-2016 or pre-2025 guidance. Regularly updating protocols and documentation to align with current recommendations helps mitigate exposure. - Educate legal teams on terminology shifts
Defense attorneys and risk management professionals must understand that terminology change does not inherently increase liability—but failing to adopt updated, consensus language could signal care gaps.
Why This Matters To You
The NPUAP’s 2016 shift from “pressure ulcer” to “pressure injury,” with expanded staging categories, remains legally significant in 2025. It underpins current standards, supports precise documentation, and informs ongoing risk management—and now serves as a foundation for the living guideline model. Legal professionals, clinical risk managers, and healthcare administrators must ensure terminology accuracy, embed device-related staging categories, and stay current with evolving guidelines to safeguard patient care and minimize liability.
By anchoring documentation and training in the authority of the 2016 revisions—and actively adapting to ongoing updates—providers can align with the standard of care and strengthen their legal defenses in contemporary pressure-injury cases.
KBD Attorneys: Advocating for the Vulnerable
At KBD Attorneys, we fiercely represent victims of nursing home abuse, group home neglect, and systemic failures across the United States. Our mission is clear: pursue justice, demand accountability, and drive meaningful reform.
Reach out today for a free and confidential consultation.
References
Ayello, E. A., Lobo, G. M., & Sibbald, R. G. (2017). Survey results from Canada and some Latin America countries: 2016 National Pressure Ulcer Advisory Panel changes in terminology and definitions. Advances in Skin & Wound Care, 30(2), 71-76.
Kottner, J., Cuddigan, J., Carville, K., Balzer, K., Berlowitz, D., Law, S., … & Haesler, E. (2020). Pressure ulcer/injury classification today: An international perspective. Journal of Tissue Viability, 29(3), 197-203.
Gould, L. J., Alderden, J., Aslam, R., Barbul, A., Bogie, K. M., El Masry, M., … & Yap, T. L. (2024). WHS guidelines for the treatment of pressure ulcers—2023 update. Wound repair and regeneration, 32(1), 6-33.
Black, J., Cox, J., Capasso, V., Bliss, D. Z., Delmore, B., Iyer, V., … & Ayello, E. A. (2023). Current perspectives on pressure injuries in persons with dark skin tones from the National Pressure Injury Advisory Panel. Advances in Skin & Wound Care, 36(9), 470-480.